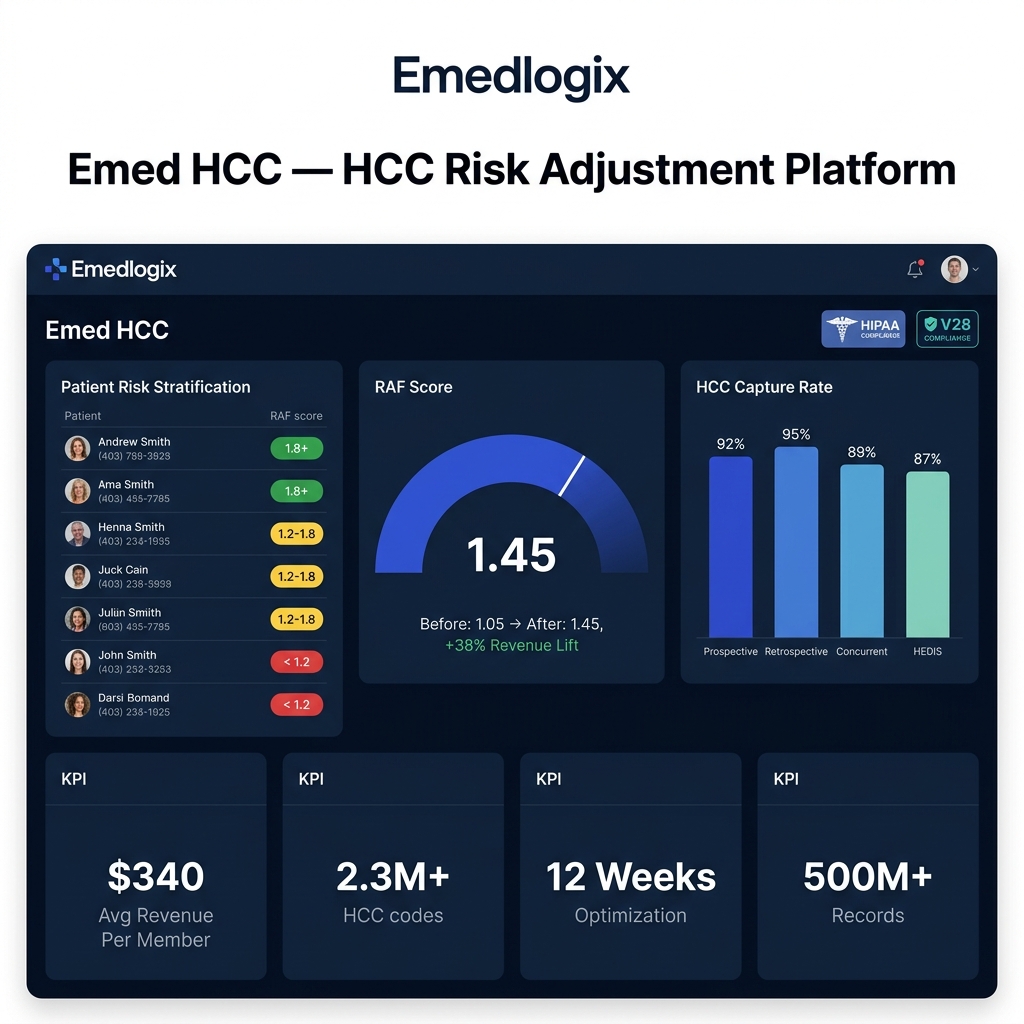
HCC Performance Analytics
Real-world outcomes from Emed HCC deployments across 50+ health plan and provider organizations.
▪ Average RAF Score Achieved
▪ HCC Capture Rates by Review Type
* Based on avg. across 50+ health plan deployments (2023-2024)
▪ Revenue Impact Metrics